An important update is available for FreeStyle LibreLinkØ. Check here for more information.
 Menu
Menu
04 Feb 2020

|
While antibiotic-resistant bacteria in the microbiome have dominated headlines, research groups have built a solid case that our microbiomes have a more macro impact on health. One such group is the Koren Lab at Bar Ilan University (Galilee, Israel), whose members have shed light on the myriad ways that microbiota and host interact to influence health and behavior. In this blog article, we shine the spotlight on two of their recent publications that used a well-established 16S ribosomal DNA (rDNA) gene sequencing protocol (powered by our PrimeSTAR Max DNA Polymerase) to investigate the impact of the microbiome on autism and pregnancy.
The quickest way to the brain is through the gut
In recent years, a proposed gut-brain axis has gained steam as a promising, novel way of understanding behavior and central nervous system (CNS) disorders through interactions between gut microbiota and the host CNS. Intriguingly, several prior studies have demonstrated microbiotal dysregulation in patients with autism spectrum disorder (ASD).
To investigate the role of the microbiome in ASD, the Koren lab employed the Shank3 (an ASD-associated gene) knockout mouse model (Tabouy et al. 2018). Microbial DNA was extracted from stool samples from male and female WT and Shank3 KO mice, and then the V4 region of the 16S rDNA gene was amplified using our high-fidelity PrimeSTAR MAX DNA Polymerase and subjected to sequencing.
Researchers noted dysregulation of several genera, but particularly noted the significant decrease in Lactobacillus species. These changes were associated with reduced GABA receptor gene expression. Treating Shank3 KO mice with L. reuteri was found to be sufficient to increase GABA receptor RNA and protein levels and reversed autism-like behavioral deficits observed in Shank3 KO mice, including social interaction (in males only) and repetitive behavior (in both sexes).
Why is this important?
Neurodevelopmental disorders such as ASD are extraordinarily complex and incompletely understood. The research presented here reveals not only host genome-induced microbiotic dysregulation, but that treatment with one species of dysregulated gut bacteria can help to reverse behavioral deficits. This demonstrates the gut microbiome can influence traits as complex as behavior, opening a novel avenue for inquiry into CNS disorders.
Bacteria, babies, and (micro)biomes
While large-scale changes in microbiota have been observed in pregnancy, their causes are not well understood. As prior work has demonstrated that the gut microbiome can influence aspects of pregnancy (e.g., weight gain and inflammation), the Koren lab opted to investigate the mechanisms of these changes (Nuriel-Ohayon et al. 2019).
Using the previously described 16S rDNA gene sequencing method, the researchers initially identified the dysregulation of multiple genera of gut bacteria, including a significant increase in Bifidobacterium, in stool samples from late-pregnancy women and female mice.
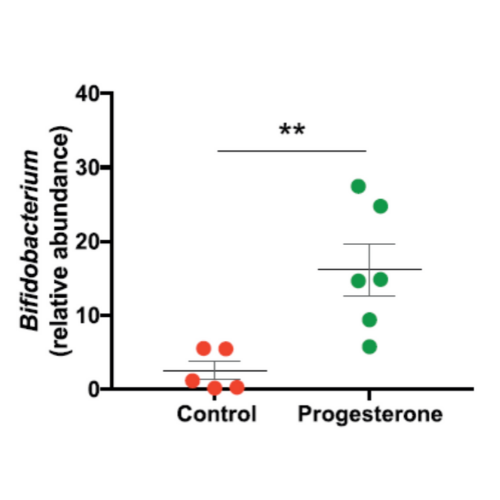
To identify the putative role of progesterone's influence on the microbiome, mice were implanted subcutaneously with either progesterone or placebo pellets. Stool samples from progesterone-treated mice demonstrated a significant increase in Bifidobacterium compared to placebo controls. The researchers then investigated the putative mechanism of this microbiotic change by adding either progesterone or PBS to stool from female mice, revealing a significant increase in relative Bifidobacterium abundance in progesterone- versus PBS-treated samples (Figure 1).
|
 |
|
Figure 1. Treatment of stool with progesterone reveals a significant increase in the relative abundance of Bifidobacterium. Image from Nuriel-Ohayon et al. 2019 and used under CC BY 4.0.
Why is this important?
Pregnancy is not only associated with significant changes to our microbiome, but these changes may play a role in determining pregnancy outcomes and neonatal health. Reduced Bifidobacterium has been associated with preterm birth (Dahl et al. 2017) as well as certain disease states in newborns (Ruiz et al. 2017). Understanding the mechanisms by which pregnancy changes the microbiome (and vice versa) will help us better understand how to identify and improve adverse pregnancy outcomes.
Amplifying the future of microbiomic health
Recent advances by researchers have vastly expanded our understanding of the microbiome's role in health and disease, but there are still challenges to surmount. Microbiomic sample complexity is extremely high, which requires high-fidelity PCR and can render amplification of starting material difficult. However, as the Koren lab's work amply demonstrates, our PrimeSTAR Max DNA Polymerase is more than up to the challenge.
References
Dahl, C. et al. Gut microbiome of mothers delivering prematurely shows reduced diversity and lower relative abundance of Bifidobacterium and Streptococcus. PLoS One 12, (2017). Nuriel-Ohayon, M. et al. Progesterone Increases Bifidobacterium Relative Abundance during Late Pregnancy. Cell Rep. 27, 730–736.e3 (2019). Ruiz, L., Delgado, S., Ruas-Madiedo, P., Sánchez, B. & Margolles, A. Bifidobacteria and their molecular communication with the immune system. Front. Microbiol. 8, (2017). Tabouy, L. et al. Dysbiosis of microbiome and probiotic treatment in a genetic model of autism spectrum disorders. Brain. Behav. Immun. 73, 310–319 (2018). |
If you enjoyed reading our articles, why not sign up to our blog mailing list? You'll get new articles straight to your inbox as they're released!